
Image: Aditya Irawan/NurPhoto via AP Images
Shortly after the pandemic began, Kelly Allison started hearing more and more professional chatter about a worrying increase in hospitalizations for eating disorders. “It was a big topic of conversation,” says Allison, who runs Penn’s Center for Weight and Eating Disorders. The media had also begun reporting on this trend.
Around the same time, a group of researchers from Penn Medicine’s Center for Health Care Innovation (CHCI), the Leonard Davis Institute, and the research arm of United Health Group had begun trying to answer questions about health care utilization during the pandemic. “We were really looking for ways in which care patterns were changing,” says David Asch, CHCI executive director.
The number of eating-disorders admissions stood out, so the research team asked Allison for help in interpreting and contextualizing the data.
They had stumbled upon something significant: From January 2018 to December 2020, these hospitalizations had doubled nationally, predominantly for anorexia and bulimia, and the length of stay had also increased by about 50%, from eight days, on average, to 12. Yet the same metrics for other common behavioral health conditions—depression, alcohol use, opioid use disorder—hadn’t budged.
The findings, published in JAMA Network Open in November, point to a trend that started just weeks after COVID-19 appeared in the United States and has shown little sign of slowing. The researchers can’t definitively explain why yet, though they surmise it’s a combination of factors, including the toll the pandemic has taken on mental health, an outsized focus on weight gain in parallel with constantly viewing ourselves on video calls, and even symptoms of COVID-19 itself.
They also don’t know how the pandemic will affect this patient population and these ailments for the long run. “This pandemic era is going to have some long-term impacts on the course of disease and the course of weight over the lifespan,” Allison says. “What that does for eating disorders? We just don’t know.”
Rebecka Peebles has seen the findings Allison and Asch published play out in real time at the Children’s Hospital of Philadelphia, where she is a member of the leadership team for the Eating Disorder Assessment and Treatment Program.
Pre-pandemic, the inpatient census ranged from 12 to 20; now it’s more like 18 to 28, she says. “We see more than 500 new patients a year,” she says. “We don’t have our statistics in for this past year, but it wouldn’t surprise me if it’s even higher. We certainly have experienced an increase in patient volume.”
This pandemic era is going to have some long-term impacts on the course of disease and the course of weight over the lifespan. What that does for eating disorders? We just don’t know.
Kelly Allison, co-director of Penn’s Center for Weight and Eating Disorders
One likely reason points to stress, which can trigger eating disorder behavior, according to the School of Nursing’s Ariana Chao. “During the pandemic, having a lack of routine and structure primed us in terms of our behaviors around food.” Additionally, she says, every video call offered another opportunity for people to stare at themselves.
Social media—and the unrealistic expectations they set—likely didn’t help, Allison says. “There was lots of talk all over social media and in the media itself about everyone gaining weight because we were all sitting at home. When someone has an eating disorder, talking about weight can be very triggering.”
Each person managed those inputs differently. Some overate or engaged in binge eating; others didn’t eat enough. Picky eaters potentially got pickier. “There’s been so much worry about gaining weight during COVID, getting out of shape during COVID,” Peebles says. “Many kids expressed to us that these messages made them worry enough to restrict their intake.”
Beyond the pandemic’s mental stressors, the physical stressors likely exacerbated the situation, too. For one, like all health care entities, eating disorder treatment programs had to quickly reimagine how to care for their patient populations in a way that provided adequate care but also kept everyone safe, according to the Peebles.
“A lot of programs had to go virtual. Some patients responded well, but there are patients who still need in-person care,” she says. “In terms of inpatient beds, many of the wards didn’t close but had to limit admissions. They may have had to go to single rooms rather than have roommates.”
We also now know much more about how COVID-19 physically changes the body, with symptoms like inflammation in the brain and a dulled sense of taste and smell occurring commonly. Peebles says those factors could potentially worsen an eating disorder that’s starting to develop.
“A change in your sense of taste doesn’t cause anorexia, but it can cause you to want to eat less,” she says. “When an eating disorder develops, the brain becomes more rigid and stuck. It makes people think they’re full when their body is starving, that they have energy when their body is exhausted. It disrupts normal signals of hunger, satiety, and activity in the brain.”
And because people were spending much more time in close quarters with immediate family—the college student who should’ve been away was suddenly home again, for example—family members had many more opportunities to witness the results of those disrupted signals. “It became much more likely they noticed unhealthy patterns that they might not have otherwise,” Allison says.
Will eating disorders numbers continue to grow or, as the pandemic evolves, drop back to pre-COVID levels? It’s still not clear.
At CHOP, Peebles says her program has yet to see signs of a downward trend; in fact, though she says they hope the numbers will level off, they’re preparing for this patient census to become the new normal. The data Allison and Asch originally published on went only through December 2020, but a team led by Asch is actively analyzing data well into 2021 to determine whether the trend held.
The bottom line, Chao says, is that more time needs to pass so more data can be collected. “We really need more research,” she says. “Adversity can be a long-term predictor of developing eating disorders. Even the transition back to ‘normal’ can exacerbate eating disorders. Everything is changing so rapidly. Then again, people are also resilient. It’s hard to say what the long-term implications will be.”
Kelly Allison is a professor of psychology in the Department of Psychiatry at the Perelman School of Medicine and director of the Center for Weight and Eating Disorders at the University of Pennsylvania.
David Asch is the John Morgan Professor in the Department of Medicine and Department of Medical Ethics & Health Policy in the Perelman School of Medicine, the Department of Health Care Management and Department of Operations, Information, and Decisions at the Wharton School, and executive director of the Center for Health Care Innovation at Penn.
Ariana Chao is an assistant professor of nursing in Penn’s School of Nursing.
Rebecka Peebles is an adolescent medicine specialist and co-director of the Eating Disorder Assessment and Treatment Program at the Children’s Hospital of Philadelphia.
Michele W. Berger

Image: Aditya Irawan/NurPhoto via AP Images

nocred
Image: Michael Levine
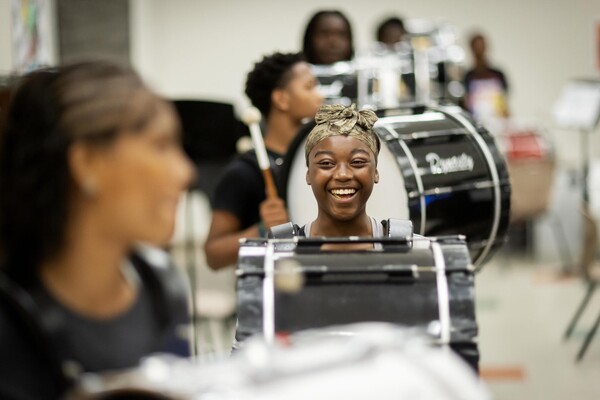
A West Philadelphia High School student practices the drum as part of a July summer program in partnership with the Netter Center for Community Partnerships and nonprofit Musicopia.
nocred